If you have AuDHD, you probably already know the feeling: your brain wants predictability and novelty at the same time. You crave a routine that works, and then you’re bored with it by Wednesday. You need things to stay the same, and you also need them to change immediately.
That contradiction is not a personality flaw. It’s what happens when autism and ADHD exist in the same person, pulling executive function in two directions at once. And it’s the reason so much standard advice for either condition alone falls flat for people with both.
This article is about the mechanics of that collision. Not just what AuDHD is, but how it specifically affects the way you plan, start tasks, handle transitions, and regulate emotions. If you’ve been trying to follow advice that was built for one condition and wondering why it keeps breaking down, the executive function piece is probably the missing context.
(A quick note before we get into it: this is educational content about a lived experience, not a clinical evaluation. If you’re working through any of this with a professional, treat this as a supplement, not a substitute.)
TL;DR
AuDHD is what happens when autism and ADHD share one brain. Here’s the practical version.
- AuDHD is a community term for co-occurring autism and ADHD, not a clinical label, but it describes a well-documented overlap where an estimated 50–70% of autistic people also have ADHD
- The core experience is often a “tug of war” between the ADHD drive for novelty and the autistic need for routine
- Executive function takes the biggest hit, with task initiation, flexibility, emotional regulation, and planning all facing pressure from both sides
- Single-condition approaches often need adjustment when both are present; hybrid approaches that build novelty into structure tend to land better
- Support that addresses both conditions at once, rather than treating them as separate concerns, makes a real difference
What AuDHD Actually Means
AuDHD is a term the neurodivergent community created to describe what it’s like to have both autism and ADHD. It’s not a formal clinical label. If someone has been formally identified with both, their paperwork will list them as separate conditions. But the term exists because the experience of having both is different enough from having either one alone that people needed a word for it.
The co-occurrence is far more common than most people realize. Research published in Frontiers in Psychiatry estimates that 50–70% of autistic people also meet the criteria for ADHD, though the exact numbers vary depending on the study and how co-occurrence is measured. A 2025 analysis of 2.4 million U.S. health insurance records found that only 1.7% of adults with ADHD had a co-existing autism identification on file. The gap between how common the overlap actually is and how often it gets formally recognized is enormous.
Part of the reason for that gap is historical. Before 2013, the DSM (the reference manual used for clinical identification in the U.S.) did not allow someone to be identified with both autism and ADHD. If you had one, you couldn’t have the other. The DSM-5 removed that restriction, but clinical practice has been slow to catch up. Many adults who grew up before 2013 were only ever identified with one condition, even if both were present the whole time. A recent National Geographic feature on the overlap put it well: researchers are only now beginning to understand how common this combination really is and why it’s been missed for so long.
That’s also why so many people are discovering this overlap as adults. It’s not that the overlap is new.
It’s that the language and the permission to name it are.
The AuDHD Tug of War
Nearly every person who writes or speaks about this experience uses some version of the same phrase: it feels like a tug of war. The metaphor sticks because it’s accurate.
ADHD, broadly, pushes toward novelty. New ideas, spontaneous decisions, the pull of something more interesting than whatever you’re currently doing. Autism, broadly, pulls toward predictability. Familiar environments, consistent processes, the comfort of knowing exactly what comes next. When both are present in one person, those drives don’t cancel each other out.
They compete.
You might build a beautifully organized system for managing your week and then abandon it in five days because the ADHD side of your brain registers “same thing again” as genuinely aversive. Or you might impulsively commit to something new (a trip, a project, a social event) and then spend the next 48 hours in escalating anxiety because the autistic side of your brain wasn’t ready for a change in the plan.
The masking layer makes this even harder to see from the outside. ADHD traits can obscure autistic patterns: someone who is socially spontaneous and talkative may not look like the autistic stereotype, even if their internal experience is one of constant social calculation. Autistic structure can obscure ADHD disorganization: someone who is hyper-organized in one area of life may look like they have everything together, when the rest of their life is in freefall. This mutual masking is one reason under-recognition is so pervasive. A 2024 study found that only 16% of children who had both conditions had previously been identified with both.
The traits don’t only oppose each other, though. Some of them stack. Emotional dysregulation is common in both ADHD and autism, and in AuDHD, emotions can hit harder and be more difficult to redirect. Social difficulties show up in both, too, but for different reasons, and when those reasons layer on top of each other, social situations become exhausting in a way that neither condition alone quite explains. The American Psychiatric Association notes that this compounding effect is a big part of why having both conditions is associated with higher rates of burnout, anxiety, and depression compared to either condition on its own.
How AuDHD Affects Executive Function
Ask someone with both autism and ADHD what the hardest part of their day is, and they’ll rarely name something dramatic. It’s usually the ordinary stuff: starting a task, switching between activities, keeping a routine going, managing an emotional reaction that arrived too fast and hit too hard.
That’s executive function. It’s the set of mental processes that help you plan, start things, stay flexible, manage your time, and regulate your emotions. Both ADHD and autism affect executive function independently, and understanding what executive dysfunction looks like for each condition is useful on its own. But when both are present in the same brain, the interaction creates something that doesn’t look quite like either one. Researchers at Vanderbilt’s Frist Center for Autism and Innovation have described this as a profile that is “neurofunctionally distinct,” not simply the sum of both conditions’ challenges stacked on top of each other. A 2025 neuroimaging study found supporting evidence: people with co-occurring ADHD and autism showed brain structure patterns that were different from either condition alone.
Here’s where the tug of war gets concrete.
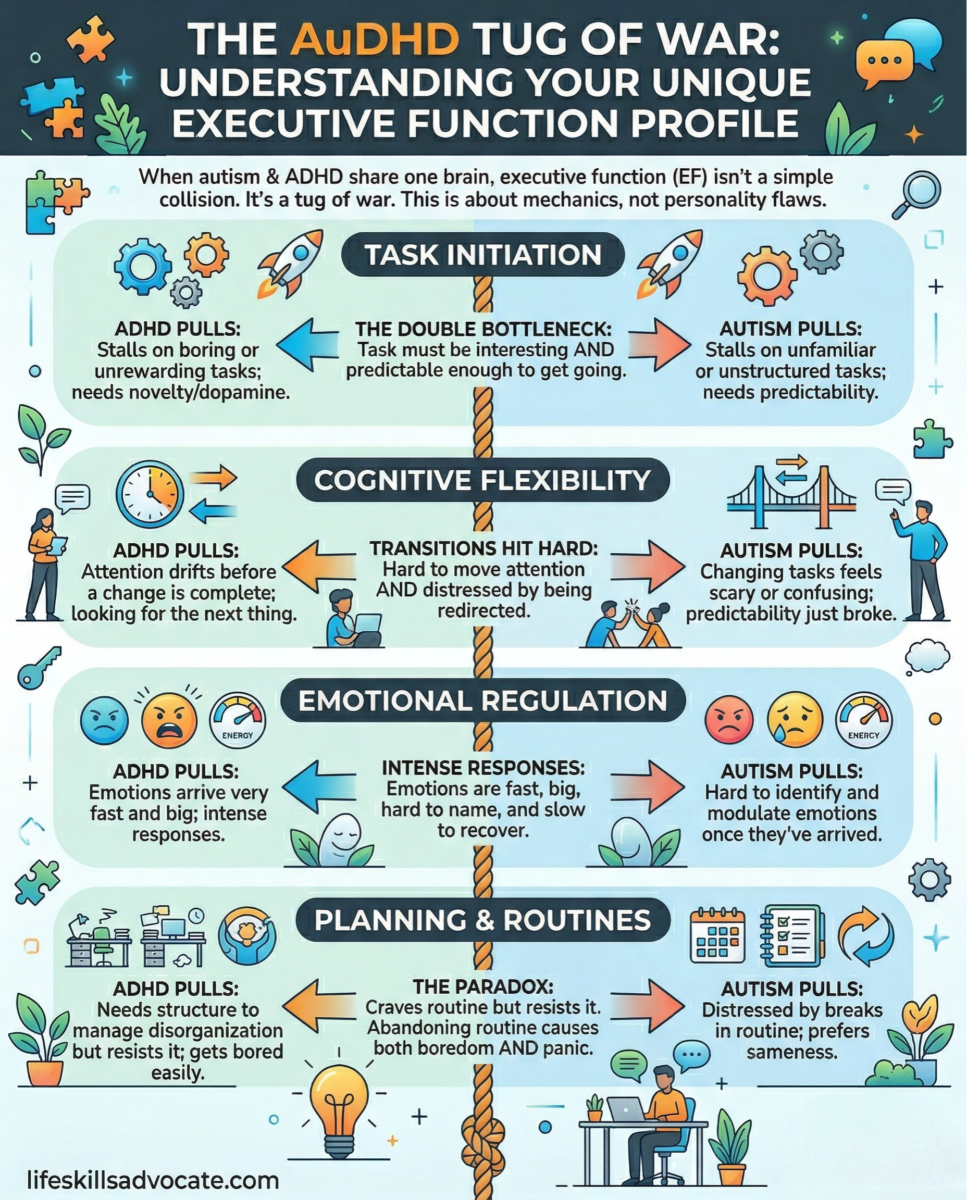
Task initiation. People with ADHD often struggle to start tasks because the brain doesn’t produce the activation signal, especially for tasks that feel boring, ambiguous, or unrewarding. People with autism often struggle to start tasks that are unfamiliar, unstructured, or require an unpredictable sequence. With both conditions present, both bottlenecks operate at once. The task might be boring AND unfamiliar. Or it might require both the dopamine hit of novelty to get started and the predictability of a known sequence to feel safe. That’s a narrow window, and when neither condition’s activation requirements are met, task initiation stalls completely.
Cognitive flexibility. Transitions, in particular, become a pressure point. ADHD makes it hard to sustain attention through the moment of switching because the brain is already scanning for the next interesting thing. Autism makes the switch itself feel threatening, because predictability just broke. AuDHD means getting hit from both sides at once: the inability to smoothly redirect attention AND the distress of being redirected at all. This is why cognitive flexibility often looks different when both are present than in either condition alone. It’s not just that transitions are hard. It’s that the reasons they’re hard are in conflict with each other.
Emotional regulation. ADHD contributes intensity and speed: emotions arrive big and fast. Autism contributes difficulty identifying and modulating emotions once they’ve arrived. Together, the result is often emotional responses that feel disproportionate to the situation and incredibly hard to course-correct. The relationship between emotional regulation and executive function is already well established for each condition separately. When both conditions share the same brain, the load on the system is higher, and the recovery time after an intense emotional response tends to be longer.
Planning and routines. This is the paradox most people with both conditions know intimately. You need structure, because without it the ADHD disorganization takes over and nothing gets done. But you also resist structure, because the ADHD brain finds predictable sequences understimulating and wants to break free. And when the routine does break, the autistic response is not just inconvenience but genuine distress. This cycle (need structure, build structure, resist structure, break structure, panic) is one of the most widely reported experiences in this population.
An important caveat: Research on how autism and ADHD interact in executive function is still emerging. Much of what we know comes from clinical observation and the lived experience of people with both conditions rather than controlled studies designed specifically for this population. That doesn’t make it less real.
It means the evidence base is still catching up to what the community has been describing for years.
AuDHD vs. ADHD vs. Autism: How Executive Function Looks Different
| EF Area | ADHD | Autism | AuDHD |
|---|---|---|---|
| Task initiation | Stalls on boring or unrewarding tasks; needs dopamine to start | Stalls on unfamiliar or unstructured tasks; needs predictability to start | Double bottleneck: task must be both interesting enough AND predictable enough to get going |
| Cognitive flexibility | Attention drifts before the switch is complete | The switch itself feels threatening or disorienting | Attention drifts AND the switch causes distress, both at once |
| Emotional regulation | Emotions arrive fast and big; hard to pause before reacting | Emotions are hard to identify and modulate once present | Emotions arrive fast, big, AND are hard to identify or redirect; longer recovery |
| Planning and routines | Routines feel boring; novelty breaks them | Routine breaks cause distress; change is aversive | Needs routine but resists it; routine breaks cause both boredom-driven abandonment and change-driven distress |
AuDHD Quick Facts
| AuDHD Quick Facts | Details | Source |
|---|---|---|
| Co-occurrence rate | An estimated 50–70% of autistic people also meet criteria for ADHD | Hours et al., 2022 |
| When dual identification became possible | 2013, with the publication of the DSM-5 | American Psychiatric Association |
| Under-recognition in adults | Only 1.7% of adults with ADHD had a co-existing autism identification in a study of 2.4 million people | Zaleski et al., 2025 |
| Under-recognition in children | Only 16% of children with both conditions had previously been identified with both | Canals et al., 2024 |
| AuDHD and executive function | Both ADHD and autism independently affect EF; the combination creates a distinct profile impacting task initiation, flexibility, and emotional regulation | Vanderbilt Frist Center, 2025; Hours et al., 2022 |
| Key internal experience | Often described as a "tug of war" between the ADHD drive for novelty and the autistic need for routine | Community and clinical descriptions |
Working With Both Brains: Practical Approaches for AuDHD
The reason so much conventional advice falls short is that it was designed for one condition at a time. ADHD advice often says to add novelty and variety to stay engaged. That can overwhelm the autistic need for predictability. Autism-focused advice often says to build rigid, unchanging routines. That can make the ADHD brain shut down from understimulation. The combination calls for a hybrid: structure that has enough flexibility built into it to keep both parts of the brain from revolting.
Anchor Activities, Not Rigid Schedules
One of the more useful reframes that comes up repeatedly in communities of people with both conditions is this: routine doesn’t have to mean schedule. What that means in practice is anchoring your day around a set of consistent conditions (the same morning drink, the same workspace, the same wind-down activity) without locking yourself into a rigid sequence or time slot. The conditions stay predictable. The order and timing can flex. This gives the autistic side its predictability and the ADHD side its breathing room.
Move the Planning Out of Your Head
Externalizing executive function is another approach that tends to work well here. Because both conditions tax internal regulation, the more you can move planning, remembering, and sequencing out of your head and into your environment, the less strain on the system. Visual schedules, phone alarms, a single capture place for all incoming tasks (one notebook, one app, one sticky-note zone), and implementation intentions (“when I finish my coffee, I will open the document”) all reduce the demand on working memory and autistic inertia.
Build Novelty Into the Container
Building novelty into structure, rather than choosing between them, is where approaches for this combination diverge most clearly from single-condition advice. Instead of varying your entire routine, you vary a small element within it. Same morning anchors, but you rotate which playlist you listen to. Same evening wind-down, but you alternate between three shows. Same work process, but you change the physical location every few days.
The container stays the same.
What’s inside it shifts just enough to keep the ADHD brain from checking out.
Check the Sensory Layer First
When nothing seems to be working and motivation has completely flatlined, checking the sensory environment before blaming yourself is almost always worth doing. Sensory overload can quietly tank executive function without announcing itself. The lights might be too harsh, the background noise too unpredictable, or the chair too uncomfortable, and those things will drain your capacity to start and sustain tasks long before you consciously register the problem. Addressing the sensory layer first, noise-canceling headphones, dimmer lighting, a different texture of clothing, can sometimes free up capacity that no amount of willpower was going to produce.
Energy accounting matters here, too. Masking uses executive function. Sensory processing uses executive function. Social interaction uses executive function. If all three are running at once (a busy workday in an open-plan office, for example), there may simply not be enough left in the tank for the task you’re trying to start when you get home.
That’s not a character problem.
It’s a resource allocation problem, and the most useful response is often to reduce demand somewhere upstream rather than trying to push harder at the point of failure.
What Executive Function Coaching Looks Like for AuDHD
A question that comes up often is whether coaching is worth it, and what it actually involves. The short answer is that executive function coaching focuses on building practical, day-to-day systems for the exact kinds of challenges we’ve been talking about: getting started on things, managing transitions, regulating energy and emotions, and keeping routines alive without burning out on them.
Coaching is not therapy, and it’s not a clinical service. It doesn’t involve processing emotional history, working through trauma, or providing medical advice. What it does involve is working collaboratively with someone to figure out which specific executive function areas are causing the most friction, and then building, testing, and adjusting external systems designed to reduce that friction. For someone with both autism and ADHD, that might mean designing a morning routine that satisfies both the need for predictability and the need for just enough variation. Or it might mean identifying which transitions consistently derail the day and putting a concrete bridge in place for each one.
What makes coaching particularly relevant when both conditions are present is the integrated approach. A coach who understands both conditions can recognize when an ADHD-oriented approach (like adding more novelty) might destabilize the autistic need for consistency, or when an autism-oriented approach (like detailed visual schedules for every hour) might create the kind of rigidity that the ADHD brain rebels against.
The goal is to find the approaches that serve both parts of the person, not just one at a time.
At Life Skills Advocate, executive function coaching is built around this kind of thinking. It’s designed for neurodivergent teens and adults, including people living at the intersection of ADHD and autism. Coaching sessions are structured around identifying what’s actually getting in the way (which is often not what it looks like on the surface), building systems that work with the person’s brain rather than against it, and adjusting those systems when they inevitably need updating. Because they will need updating. The brain that built the system last month is bored with it this month, and that’s expected, not a failure.
Coaching also tends to pair well with other forms of support. Some people work with a therapist for emotional processing and a coach for the practical systems side. Others use coaching alongside habit stacking approaches or community-based accountability like body doubling groups. There’s no single right combination. The point is that executive function support works best when it’s flexible enough to adapt as your needs change.
FAQs
Is AuDHD an official label?
No. AuDHD is a community-created term. Clinically, autism and ADHD are identified separately under the DSM-5-TR. The term captures a lived experience that the formal system hasn’t created a single category for, and it probably won’t. But the co-occurrence itself is thoroughly documented.
How common is it to have both autism and ADHD?
More common than most people expect. The most frequently cited range is that 50–70% of autistic people also meet criteria for ADHD. Going the other direction, somewhere between 15–25% of people with ADHD may also be autistic, though the true number could be higher because both conditions are still under-recognized in many groups, particularly women and people of color. A large-scale 2025 study of U.S. insurance claims found that only 1.7% of adults with ADHD had a co-existing autism identification on record, which suggests formal recognition lags far behind the actual overlap.
Does having AuDHD mean standard ADHD approaches won’t work for me?
Not exactly, but they often need adjustment. Many ADHD-oriented approaches (body doubling, externalizing reminders, breaking tasks into smaller steps) work well for AuDHD. Where things tend to break down is when the advice leans heavily on adding unpredictability to stay engaged, because that can conflict with the autistic need for consistency. Similarly, autism-focused approaches that rely on rigid, unchanging structure can backfire when the ADHD brain needs enough variation to stay activated. The sweet spot when you have both is usually keeping the structure but varying small elements within it, and paying close attention to which adjustments create relief versus which ones create a new kind of stress. If something that “should” work is making things worse, that mismatch between the approach and your specific brain is usually why.
Can AuDHD show up later in life?
Both autism and ADHD are neurodevelopmental, meaning they’re present from early in life. They don’t develop in adulthood. What does happen in adulthood, increasingly, is recognition. Many people live for decades with one identification (or none at all) before the second piece falls into place, especially people who masked effectively in childhood or were identified with anxiety or depression instead.
The research on late recognition of both conditions is still in its very early stages.
What does AuDHD executive function support look like?
The most effective support for this combination tends to address both conditions together rather than splitting them into separate tracks. That often means working with someone (a coach, a therapist, or both) who understands the specific ways ADHD and autism interact in executive function, not just the textbook version of each one individually. It also means leaning heavily on external systems: visual cues, timers, a single capture tool for incoming tasks, and environmental adjustments that reduce sensory and cognitive load. Life Skills Advocate offers executive function coaching designed for neurodivergent people living at exactly this kind of intersection.
Next Steps
If you’ve read this far and something has clicked into place, that feeling of “oh, so that’s why the usual advice doesn’t work,” you don’t need to overhaul everything at once. Start small and start specific.
- Look at the EF comparison table above and identify which area creates the most friction in your week right now. That’s your starting point, not all four at once.
- Try the free executive functioning assessment from Life Skills Advocate to get a clearer picture of where your specific EF strengths and challenges sit.
- Read more about individual EF subskills at the Executive Functioning 101 Resource Hub, which breaks each skill down with practical approaches you can try today.
- If you want 1:1 support from someone who understands how ADHD and autism interact in daily life, executive function coaching from Life Skills Advocate is built for exactly that.
Further Reading
- Hours et al. (2022): ASD and ADHD comorbidity: What are we talking about? (Frontiers in Psychiatry)
- Zaleski et al. (2025): Real-world evaluation of prevalence among adults and children with ASD, ADHD, or both (BMC Health Services Research)
- Bedford et al. (2025): Brain-charting autism and ADHD reveals distinct and overlapping neurobiology (Biological Psychiatry)
- Canals et al. (2024): Prevalence of comorbidity of autism and ADHD in school population (Autism Research)
- National Geographic (2025): Scientists are starting to understand how autism and ADHD can overlap
- American Psychiatric Association: When autism and ADHD occur together
- Vanderbilt Frist Center for Autism and Innovation: AuDHD: The hidden dynamics of a dual identification
- Life Skills Advocate: Executive dysfunction: Signs and approaches
- Life Skills Advocate: The basics of task initiation
- Life Skills Advocate: Flexible thinking skills
- Life Skills Advocate: Emotional regulation and executive function
- Life Skills Advocate: Neurodivergent burnout: Signs and recovery
- Life Skills Advocate: Autistic inertia: Start, stop, switch
- Life Skills Advocate: Habit stacking: Building consistent routines
- Life Skills Advocate: ADHD masking
