The word “meltdown” gets used loosely enough that it has lost most of its meaning. Someone loses their temper in a checkout line, and it is called a meltdown. A kid cries at a restaurant, another meltdown. But an “autistic meltdown” is something specific, and the experience does not match the way most people use the term.
An autistic meltdown is not a tantrum, not a choice, and not something that happens because someone did not try hard enough to keep it together. It is an involuntary neurological response to overwhelm, a point where the brain can no longer process what is coming in and the result is a cascade that willpower alone cannot stop.
If you have come out the other side of one wondering what just happened, or why it keeps happening, this is the explanation that does not start with a checklist written for someone else.
TL;DR
The questions people actually bring to “autistic meltdown” usually aren’t the ones a definition answers. The article works through these.
- What’s actually happening neurologically during an autistic meltdown, as opposed to what it looks like from outside?
- Why does the same trigger cause a meltdown some days and not others?
- How does an autistic meltdown differ from a tantrum in ways that change how to respond?
- What is the shame cycle that often makes the next meltdown more likely than the last one?
- What helps during a meltdown, and what tends to make it worse?
- How does recovery actually work, and how long does it usually take?
This article is educational, not medical or therapeutic guidance. If meltdowns are significantly affecting your daily life, working with a professional who understands autism can make a real difference.
What Is an Autistic Meltdown?
An autistic meltdown is an involuntary response to overwhelm. That much is straightforward. What makes it harder to explain is that the experience looks completely different from the outside than it feels from the inside.
Neurologically, a meltdown happens when the brain’s capacity to process sensory, emotional, or cognitive input reaches a hard limit. The autonomic nervous system shifts into a stress response that researchers sometimes describe as an “autonomic storm.” Heart rate spikes. Thinking narrows or stops working the way it usually does. The ability to use language, make decisions, or regulate emotions drops sharply, and these capacities tend to go offline at the same time rather than one at a time.
What that looks like from the outside varies enormously. Crying, yelling, pacing, rocking, hitting surfaces, or going completely still. From the inside, the descriptions are remarkably consistent across autistic adults: the brain is on fire, everything is too much, and there is no off switch. Both the visible and the internal version are real. Neither is a choice.
One thing most articles miss: autistic meltdowns do not always show. A 2023 qualitative study published in Autism documented what participants called “internal meltdowns,” where the full neurological overwhelm happened while external behavior stayed camouflaged. For autistic adults who have spent years masking, this pattern is familiar. The meltdown is no less intense or exhausting because it stays invisible.
Duration varies widely. Most last somewhere between 20 minutes and over an hour, but recovery extends well beyond the visible episode. That part gets its own section below.
Why Autistic Meltdowns Happen (And What Triggers Them)
Most resources list meltdown triggers as a checklist: loud noises, bright lights, unexpected changes. That is not wrong, but it misses the mechanism. Autistic meltdowns do not happen because of a single trigger in isolation. They happen because of how sensory, emotional, and cognitive load accumulates, and how the brain’s executive functions handle (or cannot handle) the total.
Sensory Overload
The most commonly recognized trigger. Fluorescent lighting, background noise that others filter out, textures, temperatures, crowded spaces. The key is not whether the input is “objectively” intense. It is whether it exceeds that person’s processing capacity on that particular day, and that threshold is not fixed. What is manageable on Monday might be unbearable on Thursday after three days of poor sleep and social demands.
Emotional and Social Overwhelm
Sensory overload gets most of the attention, but emotional and social demands are equally capable of pushing the system past its limit. Conflict, unexpected schedule changes, social interactions that require sustained masking, prolonged focus in environments not designed for the way the person’s brain works.
This is where executive functioning skills and how they connect becomes directly relevant. Emotional regulation is itself an executive function. When the EF system is already strained by task-switching, working memory demands, or cognitive flexibility challenges, the capacity to regulate emotional responses shrinks. The same conflict that might be manageable when executive function resources are fresh becomes a meltdown trigger when they are depleted.
The Buildup Effect
This is the one that confuses the people around you. You held it together through a full workday. You managed the grocery store. You got through the phone call. Then someone asks a simple question and everything falls apart.
It was not the question.
It was everything before it.
Autistic meltdowns often follow a cumulative pattern. Each demand, whether sensory, emotional, social, or cognitive, adds to a running total the brain is carrying. The final trigger can look disproportionate because nobody else can see the load that was already there. This is one of the most common reasons meltdowns get mislabeled as overreactions.
Autistic Meltdown vs Tantrum: The Difference That Matters
How can someone tell the difference between an autistic meltdown and a tantrum? The distinction matters because the response to each one should be completely different.
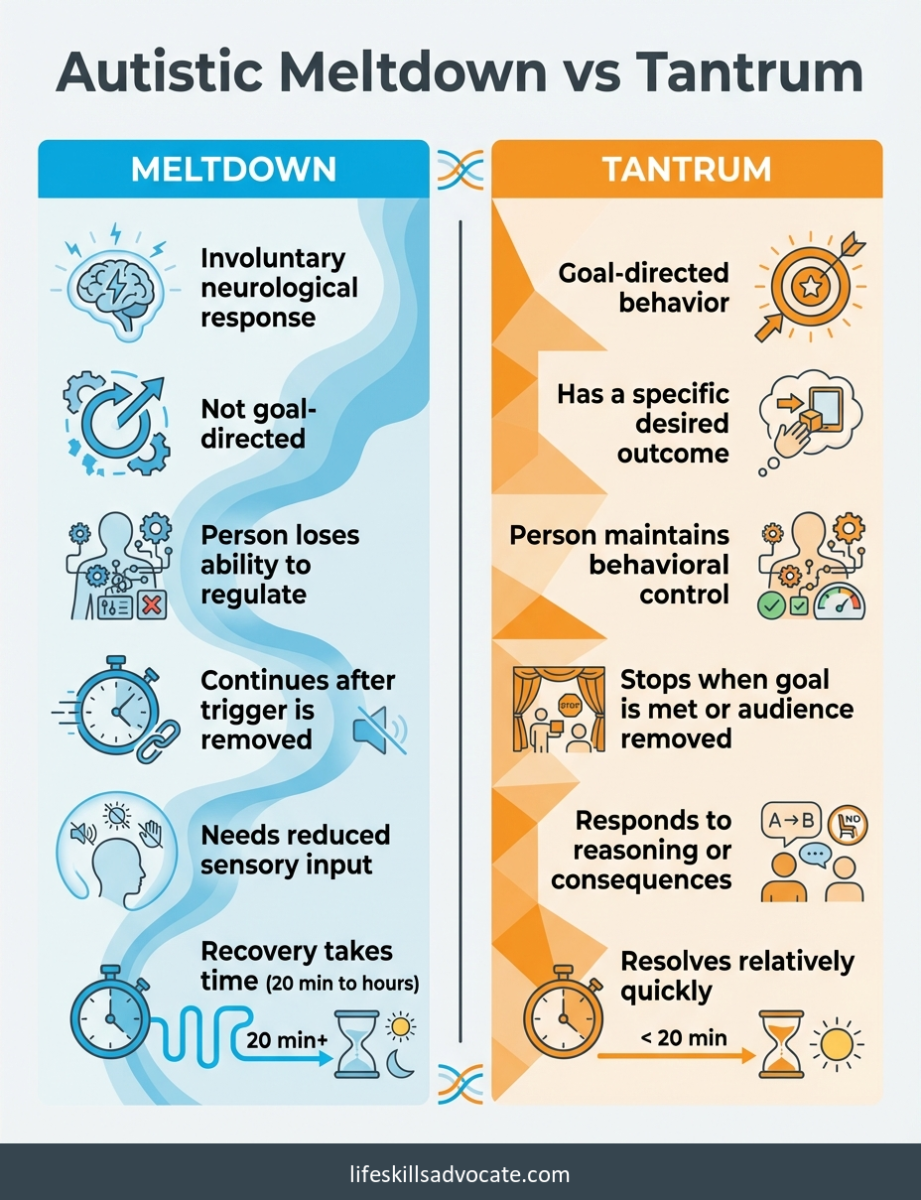
A tantrum is goal-directed. It happens because a person wants something and is using emotional behavior to get it. There is maintained behavioral control, even when the behavior looks intense. Remove the audience or meet the request, and the tantrum typically stops.
A meltdown is not goal-directed. The person is not trying to achieve an outcome. They have lost the ability to regulate their response to sensory, emotional, or cognitive overload, and the response continues even after the triggering situation is removed. Asking “what do you want?” during a meltdown usually makes things worse, because the person cannot process the question, let alone answer it.
The confusion between the two is one of the most damaging misunderstandings autistic people face. When a meltdown is treated like a tantrum, the response is exactly backward: reasoning, consequences, and social pressure add input to a system that is already overloaded. That does not de-escalate anything. It makes recovery take longer.
For autistic adults in particular, this misunderstanding compounds. Adults “should know better,” according to the expectation. The meltdown-tantrum confusion feeds directly into the shame cycle that makes the whole pattern harder to interrupt.
| Autistic Meltdown: Quick Facts | Details | Source |
|---|---|---|
| What it is | An involuntary neurological response to sensory, emotional, or social overwhelm that the person cannot control through willpower | Autism Research Institute; Lewis & Stevens, 2023 |
| Key difference from tantrum | Not goal-directed. The person does not maintain behavioral control, and the response persists even after the trigger is removed. | Autism Research Institute |
| Typical duration | 20 minutes to over an hour, with recovery time extending further. Individual variation is significant. | Reframing Autism, 2024 |
| Common triggers | Sensory overload, unexpected change, emotional stress, social exhaustion, or accumulated smaller stressors that cross a threshold | National Autistic Society |
| Who experiences them | Autistic people of all ages and support needs. Meltdowns are not limited to childhood and are well-documented in adults. | Lewis & Stevens, 2023 |
The Shame Cycle Nobody Talks About
Shame is the most common emotional response to an autistic meltdown, at least among the adults who describe their experience openly. Not frustration. Not confusion. Shame.
The pattern works like this: a meltdown happens in a context that feels socially catastrophic, at work, with a partner, in a store. The shame that follows is intense. In response, the person increases masking, performing neurotypical composure harder, suppressing more, monitoring themselves more closely. That extra effort drains cognitive and emotional resources faster. The threshold drops. The next meltdown arrives sooner. The shame deepens.
This cycle is self-reinforcing, and most guides about meltdowns skip right past it. They jump from “what triggers a meltdown” to “how to calm down,” as if the emotional aftermath does not exist. But across autism communities online, shame surfaces as the dominant experience around meltdowns, more distressing than the meltdown itself for many adults.
The shame often shows up tangled with other things: anxiety about when the next one will happen, avoidance of places or situations associated with past meltdowns, a growing sense of being fundamentally unable to handle life the way other people seem to. If any of that sounds familiar, it is worth understanding the relationship between emotional regulation and executive functioning, because the mechanisms driving the shame cycle overlap with broader EF challenges in ways that matter.
This article cannot resolve shame. But naming the cycle matters, because once it is visible as a predictable pattern and not as evidence that something is wrong with you, it becomes something you can work with rather than something that simply happens to you.
What Helps During an Autistic Meltdown
The advice most people receive about autistic meltdowns is some version of “calm down” or “remove yourself from the situation.” The problem is not that these are wrong, exactly. It is that they are directed at the wrong moment. During a meltdown, the systems that would allow someone to follow that advice are the ones that have gone offline.
What actually helps depends on which side of the meltdown you are on.
If You Are the One Having a Meltdown
The most useful thing you can do for yourself happens before the meltdown peaks: learn your warning signs. These differ from person to person, but common early signals include increased stimming, difficulty finding words, a rising sense that everything is “too much,” or the feeling of needing to escape. Some people describe it as a kind of internal pressure building with no release valve. Recognizing the early shift is what makes everything else possible.
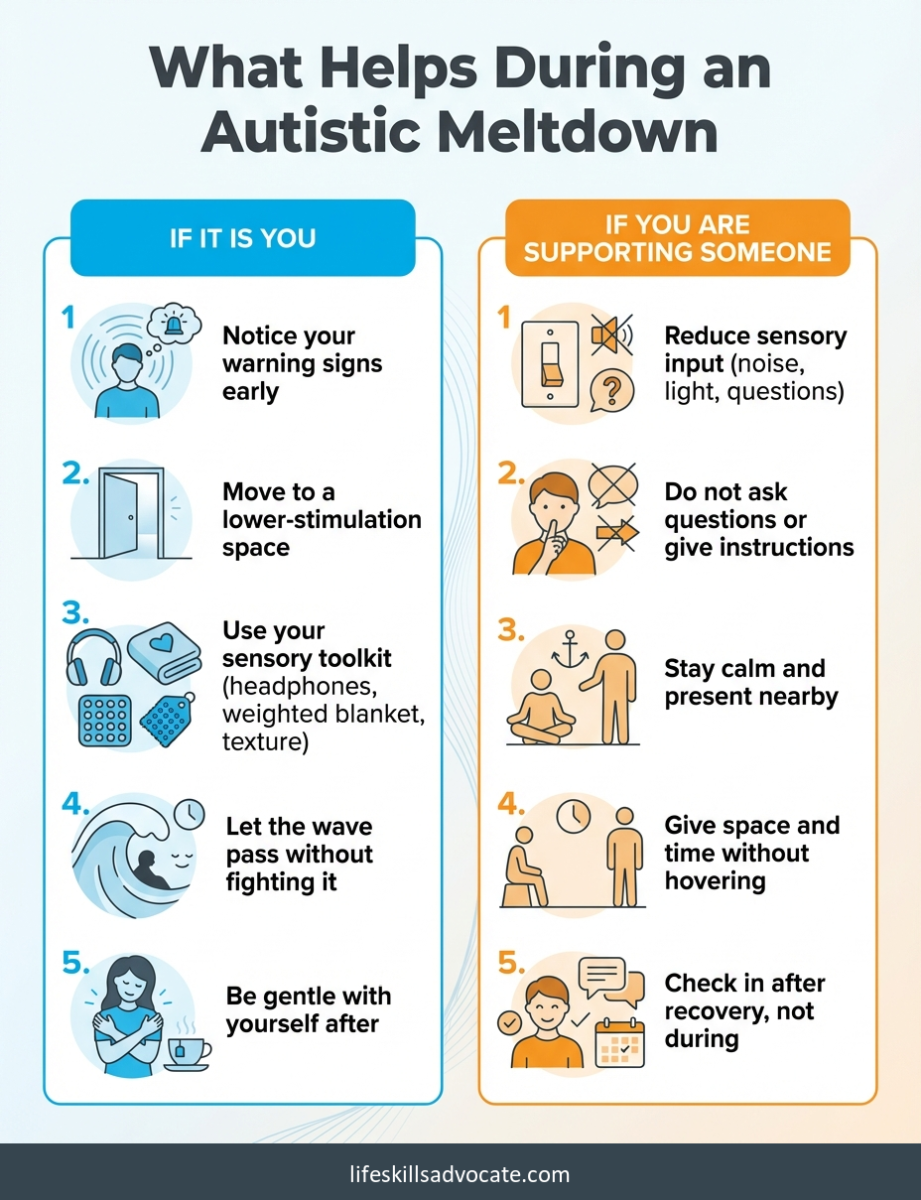
When the warning signs show up, the goal is to reduce input, not to fix the situation. Move to a quieter space if you can. Use whatever sensory tools work for you: noise-canceling headphones, sunglasses, a weighted blanket, a specific texture. If leaving is not possible, close your eyes, cover your ears, or simply stop trying to interact. Even small reductions in sensory input help. Permission to withdraw is not defeat. It is one of the most effective responses available.
If the meltdown is already happening, the only real task is to ride it out safely. It will pass. Knowing that in advance, even when it does not feel true in the moment, is its own kind of resource. The relationship between stimming and self-regulation is relevant here, because stimming during a meltdown is often the nervous system’s attempt to stabilize, not a sign that things are getting worse.
If You Are Supporting Someone
The instinct is usually to talk. Ask what is wrong, offer reassurance, suggest solutions. During an autistic meltdown, all of that adds input to a system that is overloaded. The most helpful response is to reduce. Reduce noise, reduce light, reduce questions, reduce your own visible stress.
Stay nearby if the person wants you there, but do not touch without asking. Do not take anything said during a meltdown personally. Do not try to reason, problem-solve, or debrief while it is happening. Those conversations belong to the recovery phase, not this one.
Recovery After a Meltdown
Something that rarely gets discussed is what happens after a meltdown ends. The visible episode stops, but the body and brain are still working through the aftermath. Many autistic adults describe post-meltdown recovery as something close to an adrenaline crash: physical exhaustion, emotional flatness, difficulty concentrating, and sometimes a low-grade headache or muscle soreness from the tension.
Recovery is not instant.
For some people, it takes a few hours. For others, the rest of the day is effectively gone. How long recovery takes depends on the intensity of the meltdown, how much masking was involved, whether the person had access to a low-stimulation environment afterward, and their overall stress load going into it.
The most common mistake during recovery is rushing it. Getting back to work, resuming social obligations, or pushing through as if nothing happened all increase the chance of another meltdown coming sooner. Recovery-focused perspectives from neurodiversity-affirming organizations consistently point to the same thing: rest is not optional, it is part of the process. Reduced demands, low stimulation, and gentle re-entry into normal activity are what actually work.
For the people supporting someone in recovery, the most helpful question is not “are you okay?” right after. It is checking in later, once the person has had space to come back to themselves.
Reducing Meltdown Frequency (Without Masking More)
Reducing how often meltdowns happen is possible. Eliminating them entirely is not, and framing the goal as “no more meltdowns” adds pressure that makes the problem worse.
The starting point is usually pattern recognition. Keeping a brief record of meltdowns, even just the date, context, and what the preceding hours looked like, can surface triggers that are not obvious in real time. Many autistic adults discover that their meltdowns cluster around specific environments, times of day, or types of demand rather than being random.
Once patterns are visible, the two most effective categories of change are environmental adjustments and executive function support.
Environmental adjustments mean shaping surroundings to reduce baseline load: quieter workspaces, planned recovery time after social events, predictable routines, sensory accommodations in daily environments. These are not luxuries. They are load management.
Executive function support means building the skills and systems that help the brain manage demand more effectively. That includes structured planning to reduce the number of decisions that need to be made in real time, external cues and timers to support task transitions, and deliberate routines that reduce the cognitive cost of daily life. The research on adult meltdown management consistently points toward structure and self-knowledge over suppression.
No single approach works for everyone, and any approach will have days where it does not hold.
That is expected, not a failure. The goal is reducing the frequency and intensity of meltdowns through self-understanding and adjusted conditions, not through more willpower or better masking. Those have an expiration date.
Frequently Asked Questions
What does an autistic meltdown look like in adults?
It varies widely. Some adults cry, pace, or need to leave the room immediately. Others go quiet, stim more visibly, or shut down physically. There is no single “look.” The common thread is a loss of the ability to regulate the response to overwhelming input, whether that shows externally or not.
How long does an autistic meltdown last?
Most last somewhere between 20 minutes and an hour, though the range is wide. Recovery is a separate process and can take hours or the rest of the day. Length depends on trigger intensity, accumulated stress load, and whether the person can access a low-stimulation environment.
Is a meltdown the same as a shutdown?
No. Both are responses to the same kind of overwhelm, but they express differently. A meltdown is an outward release: crying, pacing, vocal distress. A shutdown, sometimes described as dorsal vagal shutdown, is the freeze response, involving withdrawal, going nonverbal, or physically “powering down.” Some people experience both at different times.
Can you have an autistic meltdown without anyone noticing?
Yes. Research describes what some call “internal meltdowns,” where the full neurological overwhelm is happening but external behavior stays camouflaged. Autistic adults who have spent years masking can suppress visible signs while experiencing the same intensity internally. This does not make the meltdown less real or less exhausting. In some ways it is more draining, because the effort of suppression adds another layer of demand to a nervous system that is already past its limit. The physical aftermath, including exhaustion, headaches, and difficulty concentrating, is the same whether the meltdown was visible or not. If you consistently feel completely wrecked after situations that “should not have been that bad,” and there is no proportionate external reason for the crash, internal meltdowns may be part of what is happening.
Do autistic meltdowns get better with age?
It depends. Some adults develop better self-awareness about their triggers and warning signs, which can reduce frequency. Others find that adult life, with its added demands and fewer structured environments, actually increases meltdown risk. What tends to help most is not age itself but understanding: knowing what overwhelms you, having language for it, and having at least some control over your environment. The research on this is limited enough that broad generalizations do not hold well. For some people, meltdowns shift in how they present rather than disappearing.
Next Steps
If any of this sounds familiar, the starting point is not fixing anything. It is understanding what is actually happening.
- Start noticing your warning signs. What happens in your body right before a meltdown? Increased heart rate, difficulty finding words, a feeling of internal pressure? That information is the foundation for everything else.
- Build a sensory toolkit for the environments where you spend the most time. Noise-canceling headphones, sunglasses, a fidget tool, a specific texture. Keep it accessible so it is there when you need it, not buried in a drawer.
- Take the free executive functioning assessment to identify which EF areas might be contributing to meltdown vulnerability. The connection between executive function and meltdowns is real and worth understanding.
- Talk to someone who gets it, whether that is an online community, a trusted person in your life, or executive function coaching. Understanding your meltdown patterns alone is harder than it needs to be.
Working With an Executive Function Coach
If meltdowns are tied to patterns you are struggling to change on your own, executive function coaching is one option worth knowing about. EF coaching is educational and skills-focused, not therapy. It works on the practical systems that help manage sensory load, build predictable routines, strengthen emotional regulation, and develop the self-awareness that makes meltdowns less frequent and less surprising.
Executive function coaching through Life Skills Advocate is built specifically for neurodivergent teens and adults. It is not a requirement for making progress, and it is not for everyone. But for the people who find that reading about these patterns is easier than actually changing them, working with someone who understands the terrain can close that gap.
Further Reading
- The Lived Experience of Meltdown for Autistic Adults – Lewis & Stevens, 2023 (Autism journal)
- Meltdowns: A Guide for All Audiences – National Autistic Society
- Meltdowns and Calming Techniques in Autism – Autism Research Institute
- All About Autistic Meltdowns: A Guide for Allies – Reframing Autism
- 5 Ways to Deal With Adult Autistic Meltdowns – Psychology Today
- Executive Functioning 101 Resource Hub – Life Skills Advocate
- Emotional Regulation & Executive Functioning: Understanding the Relationship – Life Skills Advocate
- ADHD Stimming Explained – Life Skills Advocate
- Free Executive Functioning Assessment – Life Skills Advocate
- Executive Function Coaching – Life Skills Advocate
